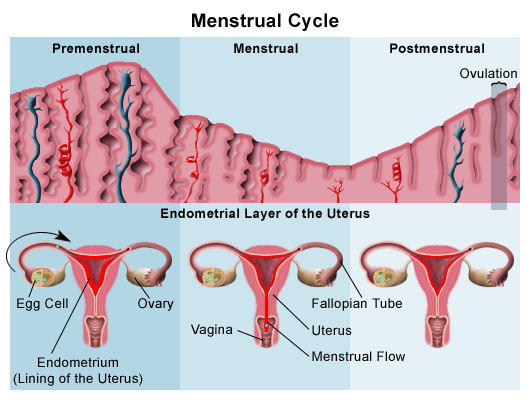
The menstrual cycle has three phases:
1. Follicular Phase (Days 1-14)This phase of the menstrual cycle occurs from approximately day 1-14. Day 1 is the first day of bright red bleeding, and the end of this phase is marked by ovulation. While menstrual bleeding does happen in the early part of this phase, the ovaries are simultaneously preparing to ovulate again. The pituitary gland (located at the base of the brain) releases a hormone called FSH – follicle stimulating hormone. This hormone causes several ‘follicles’ to rise on the surface of the ovary. These fluid filled “bumps” each contain an egg. Eventually, one of these follicle becomes dominant and within it develops a single mature egg; the other follicles shrink back. If more than one follicle reaches maturity, this can lead to twins or more. The maturing follicle produces the hormone estrogen, which increases over the follicular phase and peaks in the day or two prior to ovulation. The lining of the uterus (endometrium) becomes thicker and more enriched with blood in the second part of this phase (after menstruation is over), in response to increasing levels of estrogen. High levels of estrogen stimulate the production of gonadotropin-releasing hormone (GnRH), which in turn stimulates the pituitary gland to secrete luteinizing hormone (LH). On about day 12, surges in LH and FSH cause the egg to be released from the follicle. The surge in LH also causes a brief surge in testosterone, which increases sex drive, right at the most fertile time of the cycle.
2. Ovulatory Phase (Day 14)The release of the mature egg happens on about day 14 as a result of a surge in LH and FSH over the previous day. After release, the egg enters the fallopian tube where fertilization may take place, if sperm are present. If the egg is not fertilized, it disintegrates after about 24 hours. Once the egg is released, the follicle seals over and this is called the corpus luteum.
3. Luteal Phase (Days 14-28)After the release of the egg, levels of FSH and LH decrease. The corpus luteum produces progesterone. If fertilization has occurred, the corpus luteum continues to produce progesterone which prevents the endometrial lining from being shed. If fertilization has not occurred, the corpus luteum disintegrates, which causes progesterone levels to drop and signals the endometrial lining to begin shedding.
-The Society Of Obstetricians and Gynecologists of Canada
1. Follicular Phase (Days 1-14)This phase of the menstrual cycle occurs from approximately day 1-14. Day 1 is the first day of bright red bleeding, and the end of this phase is marked by ovulation. While menstrual bleeding does happen in the early part of this phase, the ovaries are simultaneously preparing to ovulate again. The pituitary gland (located at the base of the brain) releases a hormone called FSH – follicle stimulating hormone. This hormone causes several ‘follicles’ to rise on the surface of the ovary. These fluid filled “bumps” each contain an egg. Eventually, one of these follicle becomes dominant and within it develops a single mature egg; the other follicles shrink back. If more than one follicle reaches maturity, this can lead to twins or more. The maturing follicle produces the hormone estrogen, which increases over the follicular phase and peaks in the day or two prior to ovulation. The lining of the uterus (endometrium) becomes thicker and more enriched with blood in the second part of this phase (after menstruation is over), in response to increasing levels of estrogen. High levels of estrogen stimulate the production of gonadotropin-releasing hormone (GnRH), which in turn stimulates the pituitary gland to secrete luteinizing hormone (LH). On about day 12, surges in LH and FSH cause the egg to be released from the follicle. The surge in LH also causes a brief surge in testosterone, which increases sex drive, right at the most fertile time of the cycle.
2. Ovulatory Phase (Day 14)The release of the mature egg happens on about day 14 as a result of a surge in LH and FSH over the previous day. After release, the egg enters the fallopian tube where fertilization may take place, if sperm are present. If the egg is not fertilized, it disintegrates after about 24 hours. Once the egg is released, the follicle seals over and this is called the corpus luteum.
3. Luteal Phase (Days 14-28)After the release of the egg, levels of FSH and LH decrease. The corpus luteum produces progesterone. If fertilization has occurred, the corpus luteum continues to produce progesterone which prevents the endometrial lining from being shed. If fertilization has not occurred, the corpus luteum disintegrates, which causes progesterone levels to drop and signals the endometrial lining to begin shedding.
-The Society Of Obstetricians and Gynecologists of Canada
Menstruation
Using a Menstrual Cup
|
1. Fold and hold
Always start by washing your hands. Fold Cup using a fold that works best for you. Many start with the C-fold. 2. Insert and ensure As with tampons, gently insert the folded cup into your vagina, tilting it back to the base of your spine. The cup should sit as low as it can comfortably sit inside your vagina, normally lower than a tampon but with the stem fully inside. When the cup is inside, it will pop open, creating a light suction. The suction is how the cup prevents leaks, so use your finger to check if it is fully unfolded. Twist or rotate the cup if you need to. |
3. Use it up to twelve hours
One of the great benefits of using a menstrual cup is that it can be used for up to twelve hours. How often you need to empty your cup depends on your cycle and flow, though most menstrual cup users find they need to empty it only in the morning and again in the evening.
4. Remove and empty
With clean hands, gently pull the stem of the cup downwards until you can reach and grip the base of the cup. Pinch the base to release the suction and take it out gently.
You may need to use your pelvic muscles to push your cup lower in the vagina to help you reach the base with your fingers.
When you have removed your cup, empty it into the toilet, and rinse it with water.
If you do not have access to water, you can wipe it with some tissue or simply reinsert it directly after emptying it. But make sure to rinse it at your next available opportunity,
5. Re-insert
When your cup is rinsed, you can reinsert it, and you are ready to go again!
One of the great benefits of using a menstrual cup is that it can be used for up to twelve hours. How often you need to empty your cup depends on your cycle and flow, though most menstrual cup users find they need to empty it only in the morning and again in the evening.
4. Remove and empty
With clean hands, gently pull the stem of the cup downwards until you can reach and grip the base of the cup. Pinch the base to release the suction and take it out gently.
You may need to use your pelvic muscles to push your cup lower in the vagina to help you reach the base with your fingers.
When you have removed your cup, empty it into the toilet, and rinse it with water.
If you do not have access to water, you can wipe it with some tissue or simply reinsert it directly after emptying it. But make sure to rinse it at your next available opportunity,
5. Re-insert
When your cup is rinsed, you can reinsert it, and you are ready to go again!
© 2012-2018 Endometriosis and me